QIMA Life Sciences 有许多体外或离体模型可供您使用:
- 细胞系
- 外周血免疫细胞(PBMC 和纯化血细胞群:T 淋巴细胞亚群、单核细胞、多形核细胞等)。
- 巨噬细胞和单核细胞衍生的树突细胞
- 正常人表皮角质形成细胞 (NHEK)
- 正常人真皮成纤维细胞 (NHDF)
- 肌成纤维细胞
- 间充质干细胞
- 微血管内皮细胞
- 正常人表皮黑素细胞 (NHEM)
- 感觉神经元
- 重建人表皮 (RHE)
- 真皮替代物
- 皮肤外植体(间接体内 )
在这些模型上,我们可通过衡量以下项来评估活性化合物、制剂或医疗设备的促愈合效果。
- 炎症反应、皮肤伤口的清洁和天然免疫
- 表皮再植
- 新血管形成和神经突生成
- 合成细胞外基质、纤维化和成肌纤维细胞相互作用
- 真皮重构和表皮分化
- 色素沉着
QIMA Life Sciences 在伤口愈合和皮肤再生领域提出的所有标准测定中,有以下几个例子:





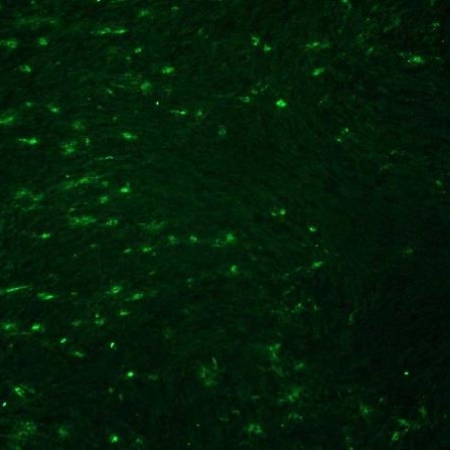
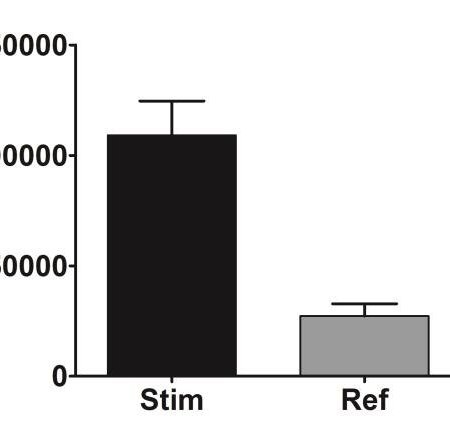
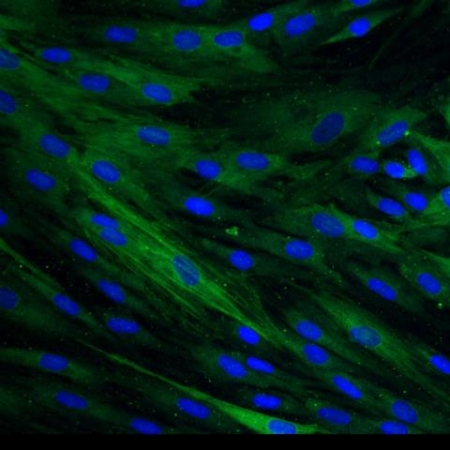
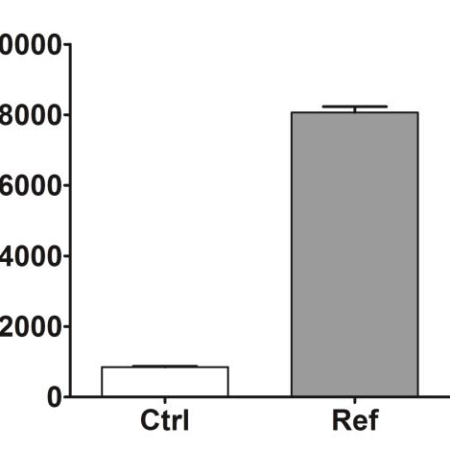
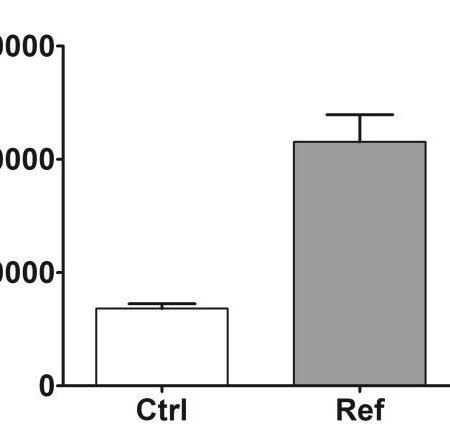
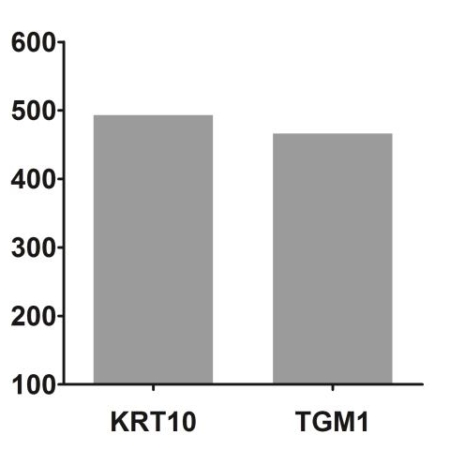
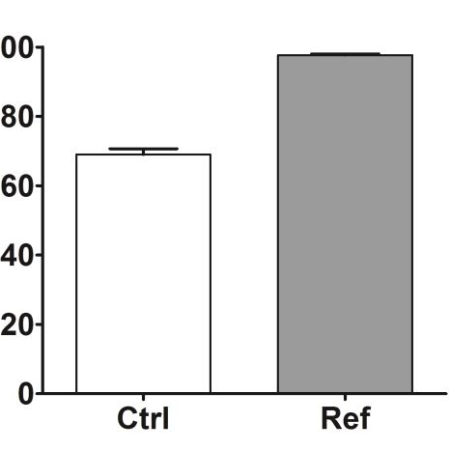
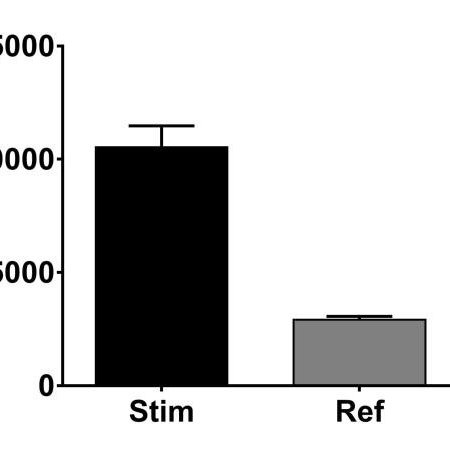



Wound healing, granulation phase and maturation phase
Wound healingThe third phase of wound healing, consisting in the replacement of the provisional fibrin matrix with granulation tissue once the wound has been debrided, includes several sub-phases: re-epithelialization, fibroplasia, collagen deposition and angiogenesis.
Wound healing, hemostasis phase and inflammatory phase
Wound healingThe inflammatory phase is characterized by the sequential infiltration of polymorphonuclear neutrophils (PMNs), monocytes/macrophages and lymphocytes. IL-8 facilitates PMNs migration from surrounding blood vessels.
Wound healing, overview
Wound healingWound healing is a complex and dynamic process of restoring skin cellular structures and tissue layers that involves multiple components: differentiated cells , stem cells , hair follicles, extracellular matrix (ECM) proteins, cytokines networks, microRNAs , blood vessels, nerves and mechanical forces.
Study of proliferation and 3D epidermal reconstruction from foreskin, auricular and trunk keratinocytes in children
Wound healingOur studies highlight the potential of foreskin tissue for autograft applications in boys. A suitable alternative donor site for autologous cell transplantation in female paediatric burn patients remains an open question in our department. We tested the hypothesis that in vitro studies and RHE reconstructive capacities of cells from different body sites can be helpful to select an optimal site for keratinocyte isolation before considering graft protocols for girls.
Epidermal healing in burns: autologous keratinocyte transplantation as a standard procedure: update and perspective
Wound healingIn the contexte of skin graft, cell suspensions transplanted directly to the wound is an attractive process, removing the need for attachment to a membrane before transfer and avoiding one potential source of inefficiency. Choosing an optimal donor site containing cells with high proliferative capacity is essential for graft success in burns.
Foreskin-isolated keratinocytes provide successful extemporaneous autologous paediatric skin grafts
Wound healingWe report a successful method for grafting paediatric males presenting large severe burns through direct spreading of autologous foreskin keratinocytes. This alternative method is easy to implement, improves the quality of skin and minimizes associated donor site morbidity. in vitro studies have highlighted the potential of foreskin tissue for graft applications and could help in tissue selection with the prospect of grafting burns for girls.
Quantitative and qualitative study in keratinocytes from foreskin in children: Perspective application in paediatric burns
Wound healingKeratinocytes from foreskin have a high capacity for division. A potential source of cells to provide coverage in paediatric burns.
Human embryonic stem-cell derivatives for full reconstruction of the pluristratified epidermis: a preclinical study
Cell and tissue engineering, Dermatology, Pharmacology, Wound healingTo assess whether the keratinocyte progeny of human embryonic stem cells (hESCs) could be used to form a temporary skin substitute for use in patients awaiting autologous grafts, we investigated the cells’ capability of constructing a pluristratified epidermis.
Cultured keratinocyte cells from foreskin and future application for burns in children
Wound healingThe keratinocytes resulting from foreskin have a high capacity of division. These cells can divide a long time before differentiation. The observations enable us to propose with our patients the keratinocytes from foreskin for wound healing especially for burns in children.
Stimulation of the proliferation of human dermal fibroblasts in vitro by a lipidocolloid dressing
Wound healingThe effect of Urgotul on normal human dermal fibroblast proliferation was studied in vitro and compared with that of two other dressing: Mepitel and Tulle Gras.