WHAT YOU WILL LEARN IN THIS ARTICLE:
- What Are Keratinocytes?
- What Are NHEK?
- How Are NHEK Obtained?
- What Are NHEK Used for?
- Example 1: NHEK in Cosmetic Testing
- Example 2: NHEK in Fundamental Research
What Are Keratinocytes?
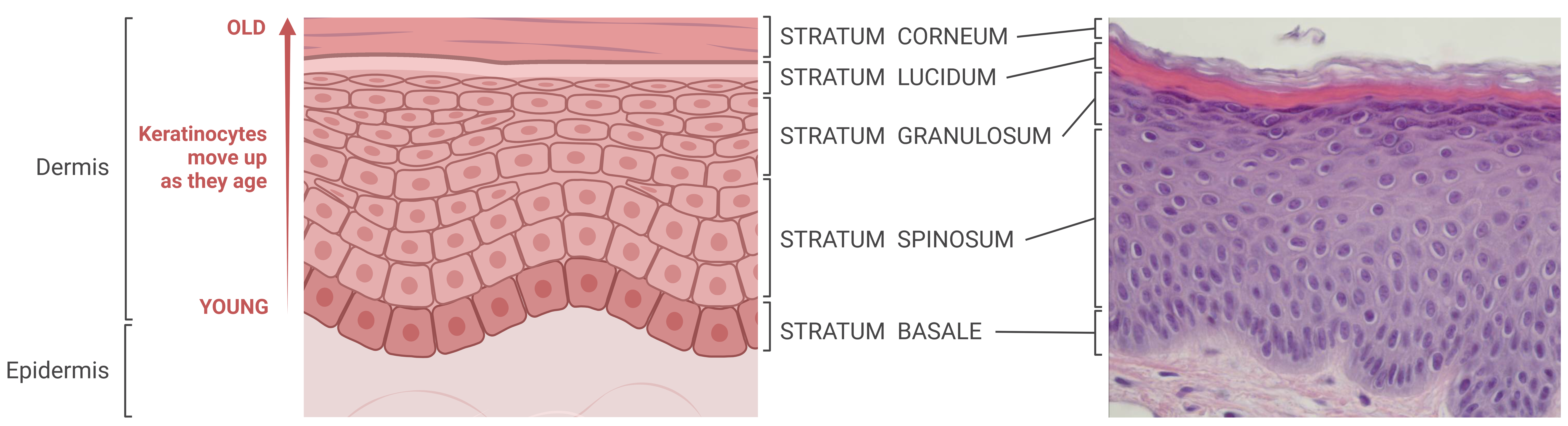
The epidermis is the most superficial layer of the skin, and its main cellular components are keratinocytes, which make up 90% of the epidermal cells. We can distinguish five epidermal sublayers according to the differentiation state of the epidermal keratinocytes (see Figure 1): the stratum basale (the innermost sublayer), stratum spinosum, stratum granulosum, stratum lucidum, and stratum corneum (the outermost sublayer).
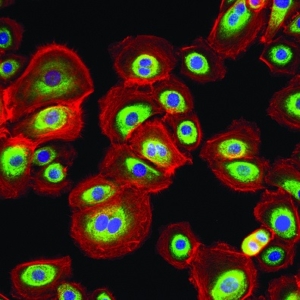
Keratinocytes from the different sublayers show morphological and physiological differences. For instance, keratinocytes in the stratum granulosum are polyhedral and contain keratohyalin granules (that’s why they are known as granular cells), whereas keratinocytes in the stratum lucidum and stratum corneum are flattened and dead. These features make it impossible to distinguish distinct boundaries between cells in the most superficial sublayers. Also important to highlight, keratinocytes in the stratum corneum, also known as corneocytes, are very different from the rest since they don’t have either nuclei or cell organelles, and are particularly important for the barrier function of the skin.
Figure 1. Schematical representation of keratinocytes in the epidermis. The epidermis comprises five sublayers; from bottom to top: the stratum basale, stratum spinosum, stratum granulosum, stratum lucidum, and stratum corneum. Other cells, such as melanocytes and Langerhans cells, are also found in the epidermis but are not included in this scheme.
Keratinocytes get their name from keratin, the major family of proteins synthesized by these cells. Keratin is a key structural protein found in hair and nails, and it can be found in some of the toughest biological materials, including animal claws, horns, and hooves. In the human skin, keratinocytes contribute to the barrier function by protecting against environmental damage and different types of stress, such as UV radiation, heat, pathogens, and water loss).
What Are NHEK?
NHEK is the acronym for Normal Human Epidermal Keratinocytes. Basically, these are keratinocytes isolated directly from the epidermis of human donors and then maintained for growth in vitro, i.e., NHEK are primary cells. They are referred to as “normal” because no skin condition or pathology was diagnosed in the patient when recovering the cells. Yet, the donor’s age can be chosen so that keratinocytes present a rather “young” or a rather “aged” phenotype.
You may also be interested in
Skin Barrier & Hydration
How Are NHEK Obtained?
Several tasks must be carried out before using NHEK in the laboratory. Indeed, following skin collection, keratinocytes are isolated, stored, and cultured.
The two main ways to procure human keratinocytes from donors are:
– to recover skin from juvenile foreskin (obtained after circumcision), or
– to recover skin from adult explants (skin remaining after plastic surgery).
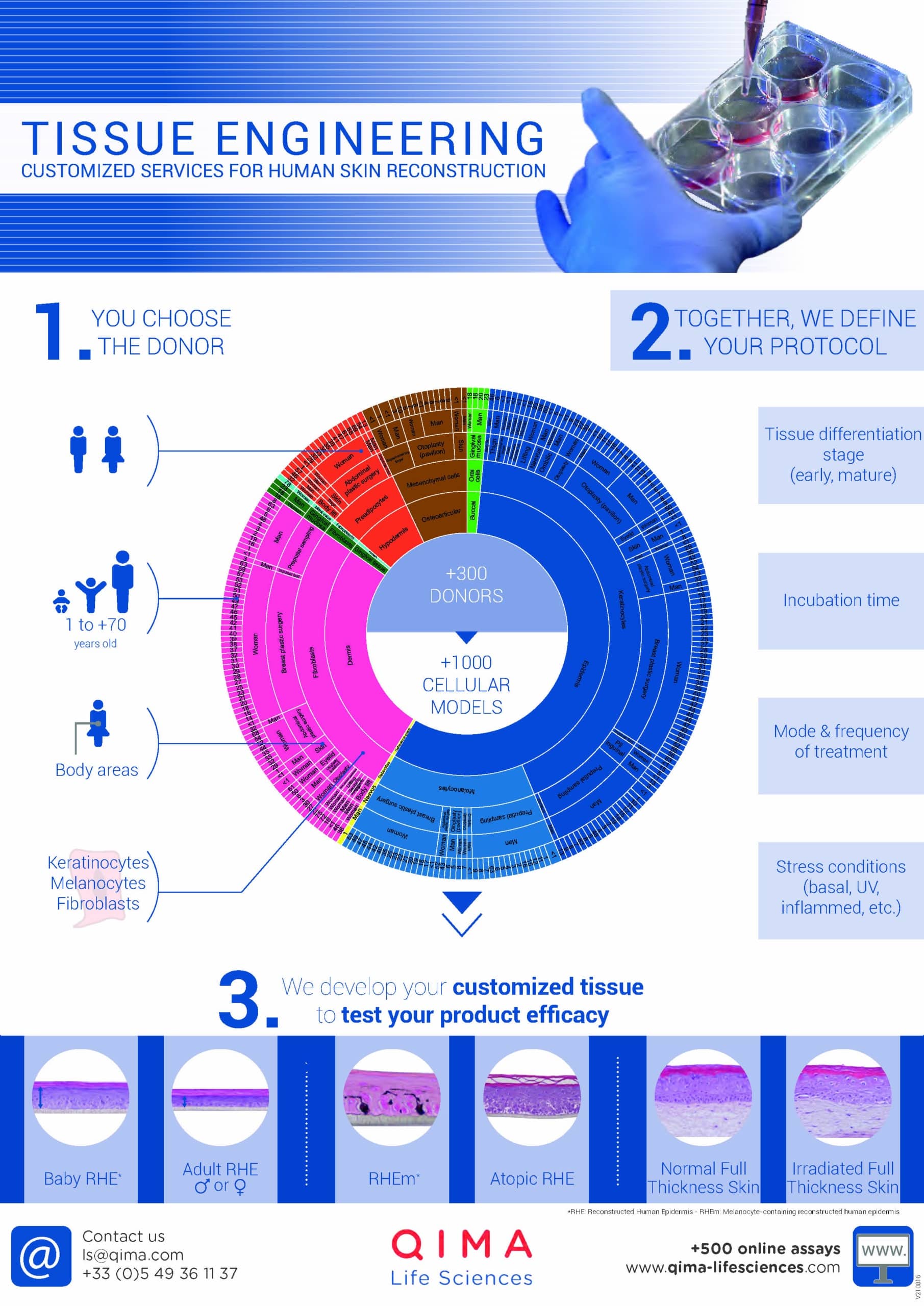
Isolation of keratinocytes from the skin is enabled by specific protocols. After this, keratinocytes are cryo-preserved (i.e., frozen) for storage. Since donors can be of different ages, sexes, and ethnicities, and explants can be recovered from different sites on the body, throughout time, it is possible to constitute a cell bank of NHEK of different characteristics. A diverse cell bank is indeed extremely valuable for different research applications.
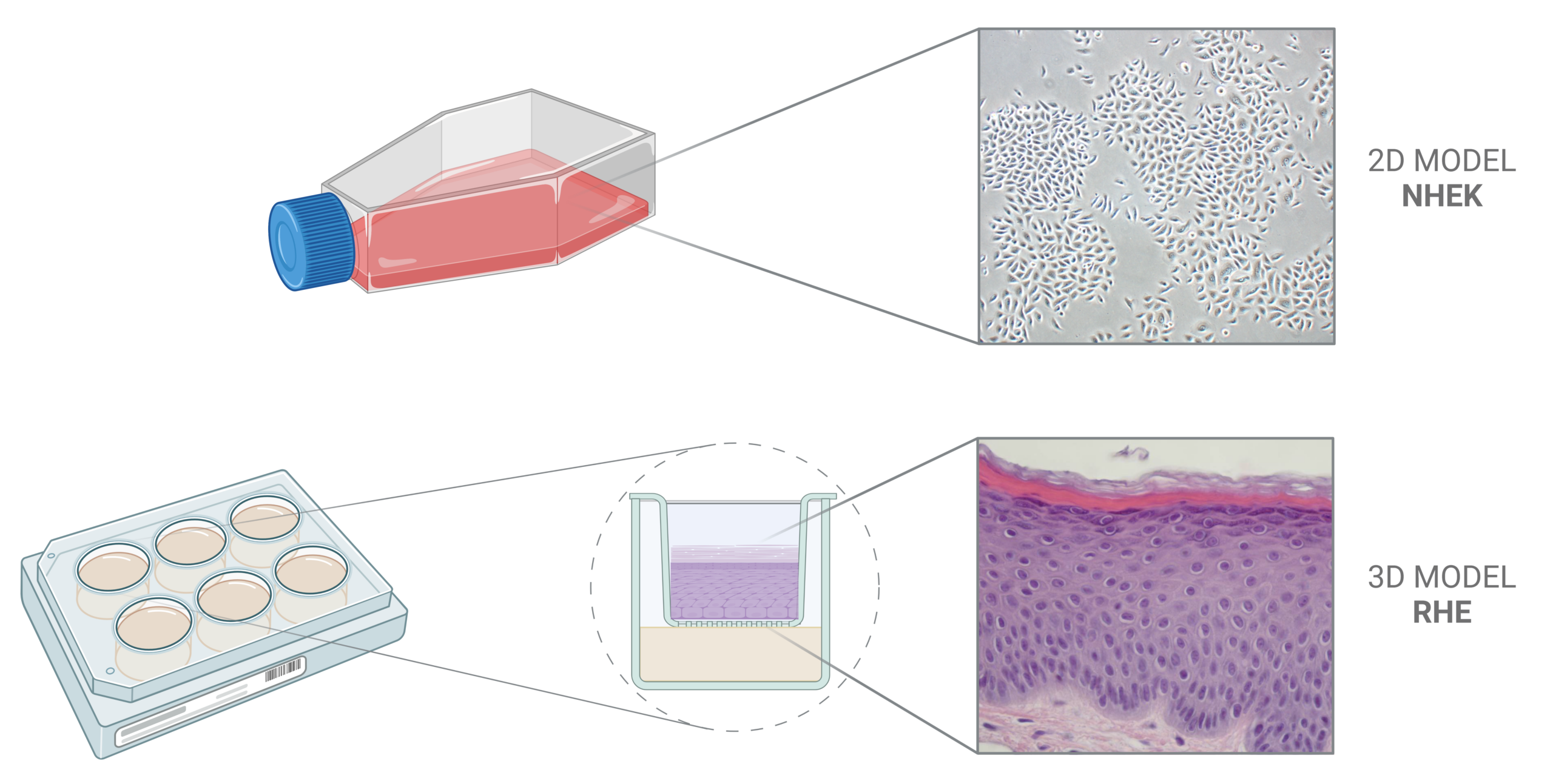
Each time NHEK are required for a given research project, an adequate number of cells will be thawed and cultured in a suitable medium. It is important to bear in mind that keratinocyte cultures can be of two types: monolayer (2D in vitro model) or multilayer (3D in vitro model). In the former case, we tend to speak of “NHEK” itself, whereas in the latter, we tend to speak rather of “RHE” or “reconstructed human epidermis”. The choice of the model will depend on the research or testing goal.
Keratinocyte monolayer cell cultures feature poor differentiation status, so they are less suitable when research targets a fully differentiated polarized tissue. However, they are particularly useful for high throughput screening, or even first efficacy tests, since they represent an easy-to-obtain and easy-to-use biological material.
Keratinocyte multilayer cell cultures feature the architecture and barrier function of a normal human epidermis. This allows the application of non-hydro-soluble compounds and final formulations, as well as the study of terminal differentiation markers. Yet, the complexity of this model makes it difficult to use for routine drug or compound evaluation.
Figure 2. Keratinocytes can be cultured in vitro either as a monolayer or as a multilayer. The 2D NHEK model is particularly useful for high throughput screening, or even first efficacy tests, because of the simplicity of obtention and use. The 3D RHE model allows the application of non-hydro-soluble compounds and final formulations, as well as the study of terminal differentiation markers, since it mimics the architecture and barrier function of a normal human epidermis.
What Are NHEK Used for?
NHEK have many different applications in research. In the laboratory, NHEK can be used to study the function and disorders of the epidermis, so their use is very common in different fields, such as cosmetology, dermatology, and toxicology.
As mentioned before, a large cell bank of NHEK enables the design of projects that better suit specific research or testing needs, since it enables the work with keratinocytes with specific and desired characteristics. Even more, although in principle NHEK derive from “normal” skin, pathological conditions (such as atopic dermatitis or psoriasis) can be mimicked in vitro by following certain protocols – many of them relying only on cytokines stimulation. Indeed, researchers have shown that inflammatory skin phenotypes are largely the consequence of the effect of cytokines on keratinocytes, thus it is possible to induce phenotypic features of different skin conditions by adding cytokines to the culture media.
Example 1: NHEK in Cosmetic Testing
-
Toxicity testing is crucial for ensuring the safety of cosmetic products and is mandatory in most consumer markets. As part of cosmetics safety testing, researchers must assess the product’s cytotoxicity, i.e., whether it is toxic to cells. The cytotoxicity assay measures the response of NHEK to the ingredients or compounds being tested by assessing the viability of cells after exposure. Being an in vitro model, NHEK offers a non-animal alternative for safety testing, particularly appreciated by markets that have banned animal testing for cosmetics (such as the European Union).
-
Efficacy testing is required to validate an almost infinite list of claims. Some examples include, but are not limited to, skin barrier and hydration, epidermal regeneration, skin firmness and cohesion, and skin microbiota balance. In this context, NHEK are of great value for in vitro efficacy testing.
Example 2: NHEK in Fundamental Research
The use of keratinocyte models is, of course, not limited to the cosmetic field. For instance, keratinocytes are a valuable model to study the pathogenesis of opportunistic microbes that are part of the normal skin microbiota. Keratinocytes have an important immunological role in the skin since they express several immune receptors against pathogen-associated molecular patterns. Thus, the NHEK model is useful, for example, to study the interaction between pathogens and skin cells in vitro.
References
Find a Research or Testing Program that Suits Your Needs
At QIMA Life Sciences, we are committed to assisting the health industry by offering competitive customer-oriented, and collaborative innovation services.
Our scientists have extensive expertise and know-how that can be applied to a wide range of pre-clinical and clinical research projects. We offer customized technical solutions that can best meet your requirements, prerequisites, and objectives, with particular attention given to the feasibility study and personalized management of your projects. With our state-of-the-art facilities and over 20 years of experience supporting projects in the dermatology, pharmaceutical, and biotechnological industries, we are pleased to offer you dedicated project management support and consulting for your R&D process.
*
Ready to discuss a testing and research program that will suit the needs of your business?